Healthcare-associated infections (HAIs) are infections that occur while receiving health care. Patients with medical devices (central lines, urinary catheters, ventilators) or who undergo surgical procedures are at risk of acquiring HAIs. HAIs continue to be a tremendous issue today, however most HAIs are preventable. The prevention and management of HAIs has advanced greatly over the last decade due to legislative, regulatory and organizational incentives. However, these changes have not resolved the gap between evidence base and clinical practice, particularly in healthcare workers’ behavioral change.
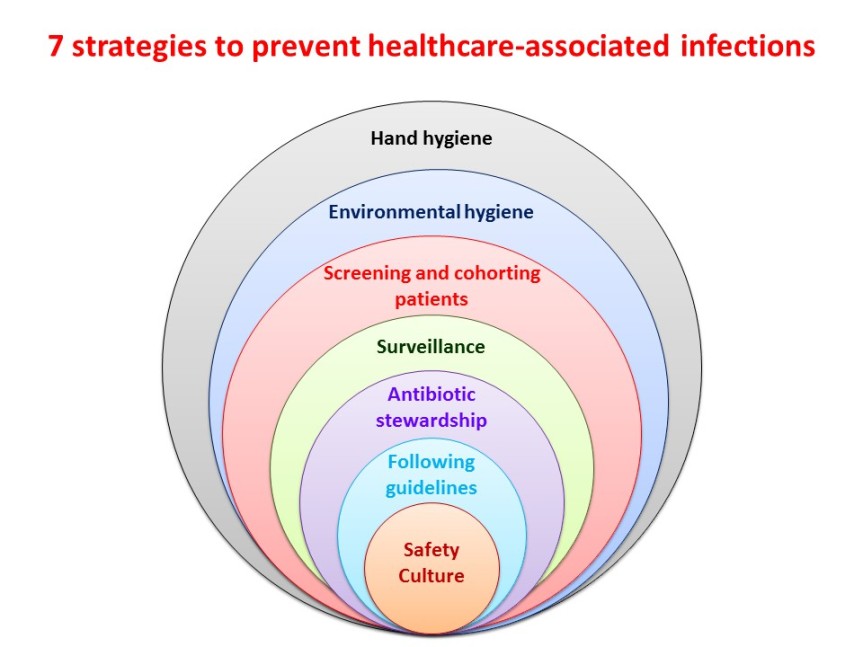
Hand hygiene
Proper hand hygiene is the most important, simplest, and least expensive means of reducing the prevalence of HAIs and the spread of antimicrobial resistance (AMR). Cleaning hands healthcare workers can prevent the spread of microorganisms, including those that are resistant to antibiotics and are becoming difficult, if not impossible, to treat.
The 5 Moments for (WHO) hand hygiene approach defines the key moments when health-care workers should perform hand hygiene.
- before touching a patient,
- before clean/aseptic procedures,
- after body fluid exposure/risk,
- after touching a patient, and
- after touching patient surroundings.
Despite acknowledgement of the critically important role of hand hygiene in reducing the transmission of pathogenic microorganisms, overall compliance with hand hygiene is less than optimal in many healthcare settings worldwide. In most healthcare institutions, adherence to recommended hand-washing practices remains unacceptably low. Hand hygiene reflects awareness, attitudes and behaviors towards infection prevention and control.
Environmental hygiene
Environmental hygiene is a fundamental principle of infection prevention in healthcare settings. Contaminated hospital surfaces play an important role in the transmission of micro-organisms, including Clostridium difficile, and multidrug-resistant organisms such as methicillin-resistant Staphylococcus aureus (MRSA) and vancomycin-resistant enterococci (VRE). Therefore, appropriate hygiene of surfaces and equipment which patients and healthcare personnel touch is necessary to reduce exposure. Wvidence supports theypothesis that hospital can act as an important reservoir of many nosocomial pathogens in several environments such as surfaces, medical equipment and water system. Healthcare settings are complex realities within which there are many critical points. Microbial contamination can result from the same inpatients, relatives and healthcare workers. The role of environmental hygiene is to reduce the number of infectious agents that may be present on surfaces and minimize the risk of transfer of micro-organisms from one person/object to another, thereby reducing the risk of cross-infection.
Screening and cohorting patients
Early detection of multidrug-resistant organisms is an important component of any infection control program. There is good evidence that active screening of preoperative patients for MRSA, with decolonisation of carriers, results in reductions in postoperative infections caused by MRSA. It has been described in patients decolonised with nasal mupirocin.
Surveillance cultures for carbapenem-resistant Enterobacteriaceae (CRE) have been advocated in a number of reports and recommendations as part of an overall strategy to combat it. Active screening for CRE using rectal surveillance cultures has been shown to be highly effective, when part of a comprehensive infection control initiative, in halting the spread of CRE in health care facilities. Isolation or cohorting of colonized/infected patients is a cornerstone of infection prevention and control. Its purpose is to prevent the transmission of microorganisms from infected or colonized patients to other patients, hospital visitors, and healthcare workers, who may subsequently transmit them to other patients or become infected or colonized themselves. Isolating a patient with highly resistant bacteria is beneficial in stopping patient-to-patient spread. Isolation measures should be an integral part of any infection prevention and control program, however they are often not applied consistently and rigorously, because they are expensive, time-consuming and often uncomfortable for patients.
Surveillance
It is widely acknowledged that surveillance systems allow the evaluation of the local burden of HAIs and AMR and contribute to the early detection of HAIs including the identification of clusters and outbreaks. Surveillance systems for HAIs are an essential component of both national and facility infection prevention and control programs. National surveillance systems should be integral to a public health system. However, recent data on the global situational analysis of AMR, showed that many regions reported poor laboratory capacity, infrastructure, and data management as impediments to surveillance.
Antibiotic stewardship
Optimal infection control programs have been identified as important components of any comprehensive strategy for the control of AMR, primarily through limiting transmission of resistant organisms among patients. The successful containment of AMR in acute care facilities, however, also requires an appropriate antibiotic use. Antibiotic stewardship programs (ASPs) can help reduce antibiotic exposure, lower rates of Clostridium difficile infections and minimize healthcare costs. Most antibiotic stewardship activities effect multiple organisms simultaneously and have as a primary goal the prevention of the emergence of antibiotic resistance. Thus, ASPs can largely be viewed in the context of horizontal infection prevention. Additionally, ASPs can contribute to the prevention of surgical site infections via the optimized use of surgical antibiotic prophylaxis.
Following guidelines
Keeping abreast of the latest findings regarding the spread of infections and strategies for prevention is essential for a successful infection prevention program.
While many infection control interventions focus on reducing the transmission of organisms, it is as important to identify measures to reduce the risk of infection. Both the World Health Organization (WHO) and the Centers for Disease Control and Prevention (CDC) have recently published guidelines for the prevention of surgical site infections (SSIs). However, knowledge, attitude, and awareness of infection prevention and control measures are often inadequate and a great gap exists between the best evidence and clinical practice with regards to SSIs prevention. Despite evidence supporting the effectiveness of best practices, many clinicians fail to implement them, and evidence-based processes and practices that are known to reduce the incidence of SSIs tend to be underused in routine practice.
Patient safety
Patient safety is described the absence of preventable harm to a patient during the process of health care and reduction of risk of unnecessary harm associated with health care to an acceptable minimum. Improving patient safety in today’s hospitals worldwide requires a systematic approach to combating healthcare-associated infections (HAIs) and antimicrobial resistance (AMR). The two go hand-in-hand. The occurrence of HAIs such as central line-associated bloodstream infections, catheter-associated urinary tract infections, surgical site infections, hospital-acquired/ventilator associated pneumonia and C. difficile infection, continues to escalate at an alarming rate. These infections develop during the course of health care treatment and result in significant patient illnesses and deaths (morbidity and mortality); prolong the duration of hospital stays; and necessitate additional diagnostic and therapeutic interventions, which generate added costs to those already incurred by the patient’s underlying disease. HAIs are considered an undesirable outcome, and as many are preventable, they are considered an indicator of the quality of patient care, an adverse event, and a patient safety issue.
