What is evidence-based medicine?
Practicing evidence-based medicine (EBM) is important in today’s healthcare environment because this model of care offers clinicians a way to achieve improved quality, improved patient satisfaction, and reduced costs.
EBM is not just about using evidence to design treatment plans; it also encourages a dialogue between patients and clinicians, so patients can share in the decision-making and make their values and preferences known. The benefit of this approach is that clinicians listen to patient concerns and take them into consideration to determine the appropriate treatment plan.
EBM includes three key components: research-based evidence, clinical expertise (i.e., the clinician’s accumulated experience, knowledge, and clinical skills), and the patient’s values and preferences.

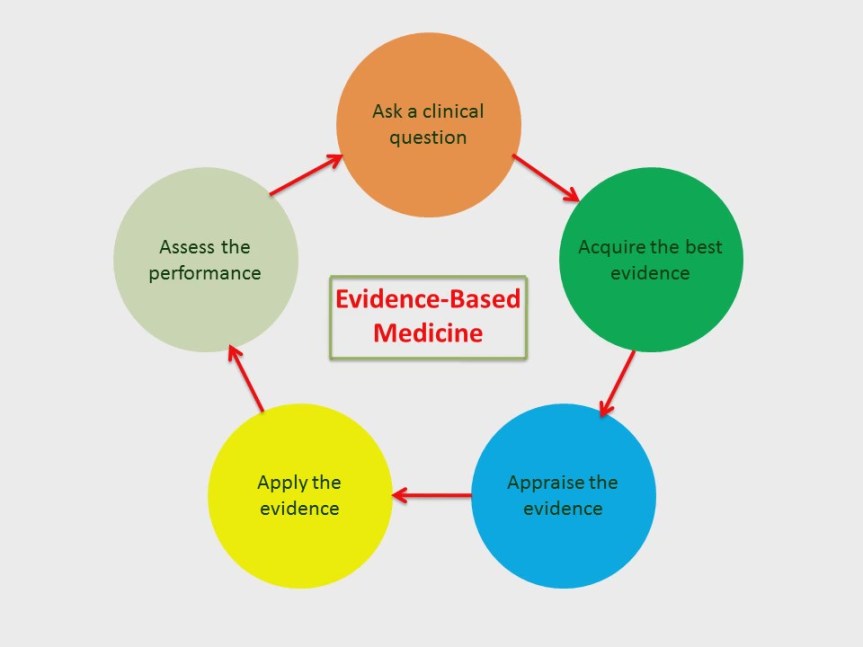
There are five steps busy clinicians can take to incorporate evidence-based medicine into their practices.
Step 1: Ask a clinical question to identify a key problem
Converting the need for information (about prevention, diagnosis, prognosis, therapy, causation, etc) into an answerable question.
Taking the time to formulate a detailed and clearly worded question is important because these words typically will be used when performing a literature search. If the question is more detailed, it is more likely that an answer will be found.
Step 2: Acquire the best evidence (medical knowledge) possible
Tracking down the best evidence with which to answer that question.
To help clinicians to compare the quality between the various sources of evidences the evidence-based medicine pyramid was designed. Within in this pyramid, evidence in the top level is the strongest because it underwent a systematic review process and meta-analysis. Evidence in the lowest level is the weakest because it is primarily based on opinions and small sample sizes, which increases room for error. Transitioning to an evidence-based model of care means encouraging clinicians to use the evidence found in the upper levels of the pyramid to see better outcomes with their patients. The following levels explain the knowledge types in each layer of the evidence-based medicine pyramid:
Level I. Evidence in Level I is considered the gold standard of medical knowledge because it comes from randomized controlled clinical trials (RCTs). The systematic review or meta-analysis of RCTs are at the top of the evidence pyramid and are typically assigned the highest level of evidence, due to the fact that the study design reduces the probability of bias.
Level II. Evidence in Level II is not considered quite as reliable at evidence from Level I, but it is still better than Level III and Level IV. Level II evidence comes from three different sources:
Controlled trials without randomization.
Cohort or case-control analytic studies.
Multiple time series studies
Level III. Evidence in Level III is based on expert opinion from experts who’ve narrowed their focus as much as possible about a complex area. The downside is that sample sizes are usually too small and there aren’t any control groups. This leaves a large margin for error unless group statistical techniques are used to compile the opinions of many experts.
Level IV. Evidence in Level IV is based on personal experience. This is the least desirable source of evidence and lacks any statistical validity.
Step 3: Appraise the evidence (make sure it’s applicable to the population and the question asked)
Critically appraising that evidence for its validity (closeness to the truth), impact (size of the effect), and applicability (usefulness in our clinical practice).
To determine the evidence’s validity, a team of clinicians should review the knowledge in question. The team can then determine if the evidence is valid (i.e., accurate) and applicable (i.e., useful for the situation or population being considered).
Step 4: Apply the evidence to daily clinical practice
Integrating the critical appraisal with our clinical expertise and with our patient’s unique biology, values and circumstances.
If the evidence passes the appraisal step and adds value to the practice of medicine, then clinicians can incorporate the new knowledge into their daily clinical practice. It’s important to note that evidence-based medicine doesn’t replace a clinician’s expertise or judgment. Its purpose is to enhance their ability to make better care decisions based on the needs and preferences of the patient.
Step 5: Assess your performance
Evaluating our effectiveness and efficiency in executing Steps 1-4 and seeking ways to improve them both for next time.
This can be accomplished by establishing a baseline and then measuring improvements. This is an ongoing process-reassessing and re-measuring any gains or losses should be part of an ongoing cycle to ensure the best outcomes.
Why evidence-based medicine?
Evidence-based medicine helps health systems achieve all three [triple] aims at once: care, health, and cost.
EBM helps clinicians stay current on standardized, evidence-based protocols. There’s an explosion of scientific knowledge being published, making it difficult for clinicians to stay current on medical best practices.
EBM uses near real-time data to make care decisions. Healthcare staff now has better access to data and more knowledge because of improved technology, such as electronic medical records (EMRs), decision support systems, built-in protocols, data warehouses, and sophisticated analytics. With this improved access to healthcare data, staff can use evidence-based medicine to provide better patient care based on near real-time data.
EBM improves transparency, accountability, and value. Payers, employers, and patients are all driving the need for the healthcare industry to show transparency, accountability, and value (e.g., high quality and safe care at the lowest possible cost). Practicing evidence-based healthcare can help the industry achieve these goals.
EBM improves quality of care. With evidence-based medicine, care improves because clinicians have access to previously untapped data and best practices vetted and agreed upon by peers.
EBM improves outcomes. The most important reason for the interest in evidence-based medicine is that it works. There’s a lot of data that shows if health systems diligently use the best clinical evidence and expertise, and ensure treatments are consistent with patient values, they’ll realize better outcomes in every way.

